As the global population of individuals experiencing hair loss continues to rise annually, hair transplant surgery—an effective medical intervention for improving hair appearance—has garnered increasing attention. However, information asymmetry has given rise to numerous misconceptions about this technology. Based on clinical practice and evidence-based medicine, this article systematically addresses five typical cognitive myths to provide scientific guidance for prospective patients.
Myth 1: Post-Transplant Maintenance Isn’t Necessary?

Dynamic Management as the Cornerstone of Long-Term Efficacy
Claims by some clinics that “transplanted hair remains permanently without shedding” severely mislead consumers. Anatomically, transplanted follicles are harvested from the occipital dominant donor area (a DHT-resistant region), whose biological properties reduce post-operative shedding risk. However, the health of native hair still depends on the overall scalp microenvironment. Clinical data show that neglecting fundamental treatment for androgenetic alopecia can lead to a 23%-35% loss of native hair within three years post-surgery.
Professional medical protocols emphasize full-cycle post-operative management: medicated shampoos containing ketoconazole are recommended for inflammation control during months 1-3; low-level laser therapy (LLLT) aids hair shaft development from months 6-12; quarterly trichoscopy is advised to monitor scalp microenvironment dynamics. The American Association of Dermatology (AADA) guidelines explicitly state that hair transplants must be combined with pharmacological treatments (e.g., finasteride, minoxidil) to achieve the dual goal of “protecting existing follicles + supplementing new hair.”
Myth 2: More Severe Hair Loss Requires Immediate Surgery?
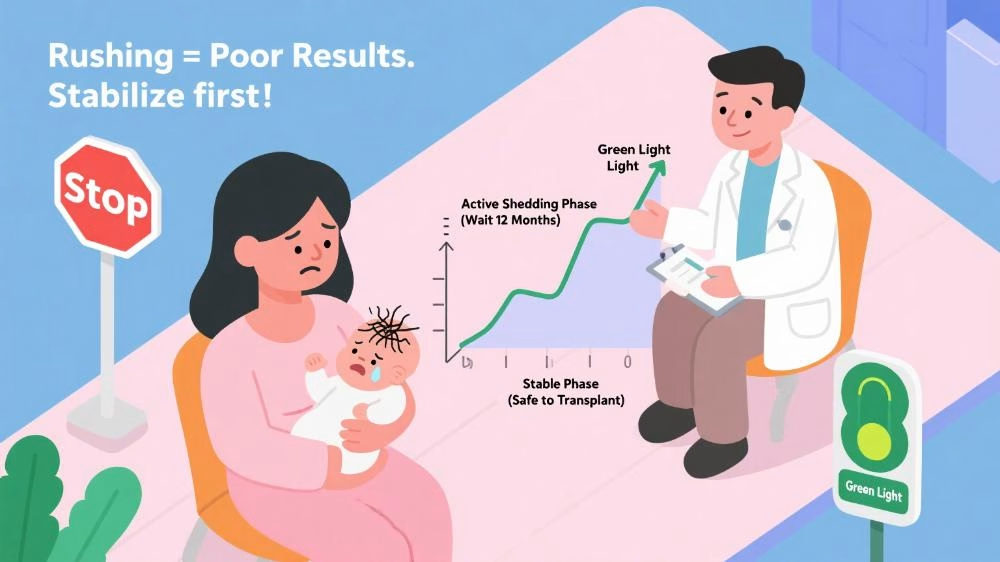
Timing the Optimal Treatment Window
Patients in acute hair loss phases (e.g., within 6 months post-partum, active alopecia areata) often rush into surgery due to anxiety. However, follicles in these stages are trapped in a pathological cycle of catagen-telogen, leading to a 40%+ reduction in graft survival rate when harvested prematurely. A 2023 study in the International Journal of Hair Restoration Surgery revealed that alopecia areata patients who waited 12 months for disease stabilization achieved a 92% follicle survival rate—significantly higher than the 58% rate during active phases.
The correct diagnostic pathway follows a “diagnose first, intervene later” principle: hormone panel testing, trace element analysis, and pull tests identify hair loss types (cicatricial/non-cicatricial, permanent/temporary). For telogen effluvium patients, 3-6 months of conservative treatment (e.g., nutritional supplementation, stress management) is advised before reassessing surgical eligibility as follicles enter the anagen phase. Clinical observations show 85% of post-partum hair loss resolves naturally within a year; hasty surgery may cause irreversible follicle depletion.
Myth 3: Donor Areas Inevitably Become Sparse?
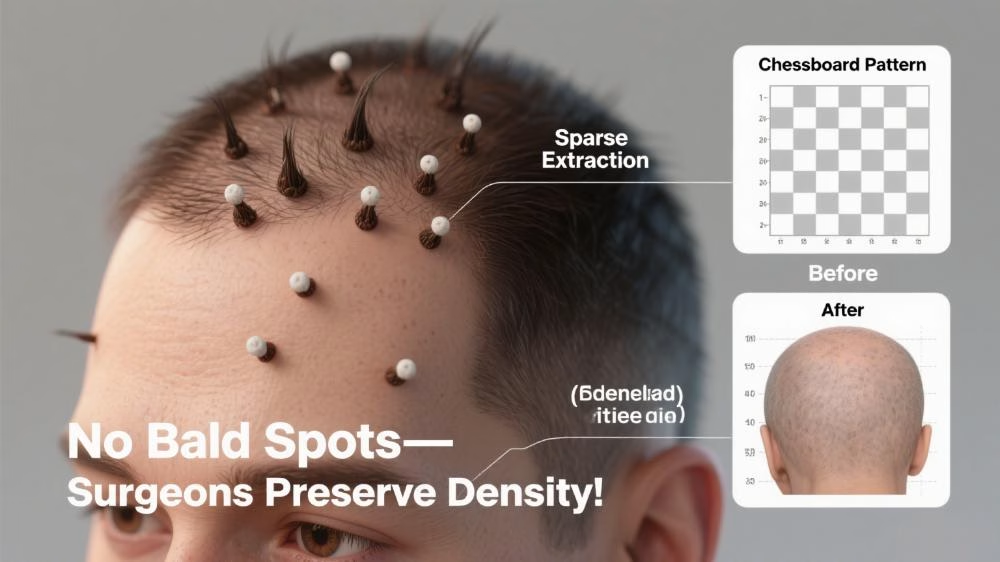
Micro-Technology Restoring Aesthetic Balance
The myth that “harvesting from the occipital area causes bald patches” stems from outdated perceptions of traditional techniques. Modern Follicular Unit Extraction (FUE) uses 0.6-0.8mm blunt punch tools with a “chessboard interval harvesting method,” restricting extraction density to 15-20 units/cm² (20%-25% of native density). Post-operative donor areas maintain natural appearance through collagen remodeling and surrounding hair coverage.
A 2024 clinical report by the Korean Hair Restoration Society (KHRS) showed that donor sites using stereomicroscopic techniques achieved an 87% follicle regeneration rate (compensatory growth in non-harvested areas) within 12 months, with scar width controlled below 0.3mm. Surgeons tailor harvesting plans based on occipital hair density (60-80FU/cm² normal range), hair diameter (60-120μm), and curvature to ensure aesthetic balance during “dense packing.”
Myth 4: Dyeing/Styling Is Prohibited After Transplant?

Scientific Care Enabling Functional Reconstruction
Misunderstandings about post-operative styling restrictions stem from misperceptions of follicle recovery phases. Transplanted hair undergoes a shedding phase (1-3 months), neogenesis (4-6 months), and reaches structural maturity at 6 months (stable keratin content in the hair cortex). Clinical trials show that gentle dyeing/perm processes (temperature ≤150℃, pH ≤9) at 6 months post-op cause no significant difference in hair diameter or cuticle integrity compared to natural hair (p>0.05).
The International Cosmetic Dermatology Hair Science (ICDHS) recommends a “three-stage protocol”: avoid chemical treatments within 3 months; choose plant-based dyes for first styling at 6 months; resume regular styling at 12 months with weekly deep conditioning using panthenol/squalane products. Note that high-temperature styling (e.g., flat irons) should not exceed 3 minutes per session to prevent thermal damage to follicle roots.
Myth 5: Hair Follicles Can Regenerate After Extraction?

Protective Utilization of a Finite Resource
As non-renewable end-organs, follicle counts are determined during embryonic development (5-10 million in adults, 2-5 million usable donor follicles in patients with alopecia). Current medical technology has not overcome follicle regeneration; a 2024 Nature Medicine review noted that while stem cell research shows promise, clinical application remains in animal trial stages. Excessive extraction (over 5,000FU per session) leads to irreversible donor site thinning and “patchy” appearance.
Standard pre-operative evaluations include 3D scalp imaging (e.g., Canfield Vectra), Trichoscan density measurement, and trichoscopic vascular analysis to ensure extraction does not exceed 30% of donor reserve. For extensive hair loss (Norwood-Hamilton Class Ⅴ+), a “staged transplantation + medication maintenance” approach is recommended: ≤3,000FU per session with 6-12 month intervals for secondary densification, maximizing follicle conservation.
Conclusion: Building a Rational Treatment Framework
The success of hair transplantation relies on precise pre-operative assessment, microsurgical techniques, and systematic post-operative care. Patients should be wary of marketing claims from non-medical entities and choose accredited clinics with Medical Institution Practice Permits and specialized hair surgeons (only 0.7% of Chinese physicians are certified by the Chinese Medical Doctor Association for hair restoration).
The International Society of Hair Restoration Surgery (ISHRS) emphasizes that any clinic claiming “universal cure” or “zero risk” violates medical principles. Prospective patients are advised to complete at least three professional consultations, review surgeons’ microsurgery certifications, and request 1-year follow-up data for over 50 cases. When confronting hair loss, rational decision-making remains the best “hair growth agent”—protecting existing follicles and scientifically supplementing new ones are equally vital.
(Data sources: International Society of Hair Restoration Surgery (ISHRS), American Academy of Dermatology (AAD), Chinese Medical Doctor Association (CMDA))


